All published articles of this journal are available on ScienceDirect.
Nasopharyngeal Airway Versus Laryngeal Mask Airway During Diagnostic Flexible Fiber-Optic Bronchoscope in Children
Abstract
Background:
Pediatric fibreoptic diagnostic bronchoscope under general anesthesia using supraglottic devices as Laryngeal Mask Airway (LMA) and Nasopharyngeal Airway (NPA) are one of the variable techniques used for patient’s ventilation during this procedure.
Objective:
We studied the effect of both devices on hypoxemia, the duration of the procedure, recovery time and the overall propofol consumption.
Methods:
Ninety patients of both sexes, aged 5-10 years, American Society of Anesthesiology Class I & II scheduled for diagnostic fibreoptic bronchoscope under general anesthesia were divided randomly into two equal groups; LMA group & NPA group, during the procedure: heart rate, non invasive blood pressure, peripheral arterial oxygen saturation (SpO2), arterial partial pressure of carbon dioxide (Pa CO2), time of procedure, recovery time and total dose of propofol were measured and compared for each patient in both groups.
Results:
Hypoxemia & desaturation incidence was more in LMA group than in NPA group with highly significant difference (p-value 0.005). Also, the duration of procedure, recovery time in PACU, and total dose of propofol consumed were significantly less in the NPA group (p< 0.001) with no difference in hemodynamic status and PaCO2.
Conclusion:
The use of NPA as supraglottic ventilating device for children undergoing diagnostic flexible fibreoptic bronchoscopy is considered a good alternative for shortening the bronchoscopy time with less incidence of hypoxemia and better recovery time compared to LMA.
1. INTRODUCTION
Pediatric bronchoscopy is defined as an endoscopic procedure to visualize the inside of the airway for diagnostic and therapeutic purposes. It is most often performed in children at the preschool age. It is obvious that bronchoscopic interventions necessitate a team approach and bring a major challenge for both the anesthesiologist and operator since they share and manage the patient`s airway [1, 2].
Various methods of airway management have been used to maintain and secure the airway, ranging from nasal canula, facemask to supraglottic devices and endotracheal tube, but choosing the most adequate method, considering the pathology and site of the lesion, the interventional procedure and the possible risks, is a major concern especially in children [3].
Supraglottic devices as laryngeal mask airway (LMA) and nasopharyngeal airway (NPA) provides the possibility of positive pressure ventilation. Furthermore, being located over the larynx permits simple entry of appropriate sized fibreoptic bronchoscope, providing the possibility of examining supraglottic and subglottic lesions along with good safety margin in securing the airway during general anesthesia and deep sedation [4].
This study aimed to compare the difference between the use of LMA & NPA as ventilating devices during diagnostic fiber optic bronchoscope in children and its role in preventing hypoxemia and its impact on the duration of the procedure, recovery time and given doses of propofol.
2. PATIENT AND METHODS
This prospective randomized single blind study was conducted on ninety patients of both genders, aging between 5 and 10 years, ASA Class I & II scheduled for elective diagnostic Flexible Fiber-optic Bronchoscope (FFB) at chest department of Ain Shams University Hospitals. Primary indications were persistent or recurrent atelectasis, pneumonia, or diffuse infiltrates and diagnostic Broncho Alveolar Lavage (BAL). The participants were enrolled from June 2016 to March 2017 after the approval of the Ethical Medical Committee and obtaining a written informed consent from their parents or guardians. Patients were randomly divided into 2 groups (forty-five in each group) using a computer-generated random number table to either laryngeal mask airway group (LMA group), or nasopharyngeal airway group (NPA group).
Exclusion criteria included parent’s refusal, ASA III or more, intrinsic and idiopathic coagulopathy, known allergy to any of the study medications, furthermore, patients were excluded if they had severe hypoxemias due to severe cardiac or lung disease.
For all enrolled patients, full history, clinical examination and routine laboratory investigations were done. Pre-induction of all patients had an IV access (22 gauge peripheral canula) using EMLA cream, premedication drugs were given in the form of midazolam 0.05 mg/kg iv, ketamine 1 mg/kg iv, dexamethasone 0.02 mg/kg iv, ondansetron 0.1 mg/kg iv & Ceftriaxon 50 mg/kg, after making sensitivity test as antibiotic prophylaxis.
General anesthesia was conducted using supraglotic devices either laryngeal mask airway (LMA group) or nasopharyngeal airway (NPA group) using open circuit (modified Ayre’s T-piece). Basic monitoring, including ECG, pulse oximetry and non-invasive blood pressure, was applied to all patients, throughout procedure and in the PACU.
After oxygenation using facemask with 100% FiO2 & sevofloran 2%, propofol 2 mg/kg IV was given. In LMA group we inserted laryngeal mask airway and connected it to modified Ayre’s T-piece then the FFB was introduced by a pediatric bronchoscopist through the LMA, while disconnecting the circuit and local anesthetic (lidocaine 3 mg/kg) it was sprayed on the vocal cord through the bronchoscope channel 2 minutes before introducing it through the vocal cords.
In the NPA group, the nasopharyngeal air way was introduced to one of the nostrils and connected to modified Ayre’s T-piece circuit using endotracheal tube connector of the same size then FFB was introduced through the mouth with the aid of a bite block away from the device, thus in NPA group, we didn’t disconnect the circuit throughout the procedure, while in group LMA we disconnected the circuit during the procedure.
Anesthesia was maintained using sevoflorane 2% in 100% FiO2 and additional IV doses of propofol 1 mg/kg per dose was titrated to deepen anesthesia to avoid child movement and coughing during the procedure when needed. Baseline arterial oxygen saturation (SpO2) together with hemodynamic parameters in the form of heart rate, systolic & diastolic blood pressure was recorded every 5 minutes throughout the procedure and in the PACU.
Episodes of Desaturation (Desaturation was defined as SpO2 < or = 90%) occurred during the procedure and lowest SpO2 were recorded and managed in both groups by halting the procedure and assisting the ventilation till SpO2 returned to normal. In LMA group, we had to reconnect the circuit; however, in (NPA) group, we only closed the mouth and the other nostril to assist ventilation.
To assess the effect of both techniques on hypoventilation, two Arterial Blood Gases (ABG) were done for each patient. The 1st one shortly after induction of anesthesia and the 2nd one at the end of the procedure before recovery and the difference between PaCO2 in the two samples were calculated and compared between both groups.
After recovery from anesthesia all patients in both groups were transferred to PACU and the time from arrival to PACU till discharge was recorded, patients were discharged by the anesthetist from PACU after fulfilling criteria of discharge (modified Aldret’s score ≥ 9). The duration of the procedure was also recorded and the total dose of propofol during the procedure apart from the induction dose was calculated.
2.1. Statistical Methods
Sample size calculation was calculated using PS (version 3.0.43, Department of Biostatistics, Vanderbilt University, located in Nashville, United States), based upon the assumption that using nasopharyngeal airway as a supraglottic ventilating device will decrease the incidence of desaturation and hypoxemia by 20% and taking power 0.8 and alpha error 0.05, a minimum sample size of 45 patients was calculated for each group.
Statistical analysis was performed using computer software statistical package for the social science (SPSS, version 20; SPSS Inc., Chicago, Illinois, USA). Description of quantitative (numerical) variables was performed in the form of mean ± SD. Description of qualitative (categorical) data was performed in the form of number of cases and percentage. Chi-square (X2) test of significance was used in order to compare proportions between two qualitative parameters, independent-samples t-test of significance was used when comparing between two means, Mann Whitney U test: for two-group comparisons in non-parametric data. The significance levels were set at P-value of 0.05 or less, and P-value of 0.01 or less, which were considered highly significant.
3. RESULTS
In this randomized, prospective, single blinded study, 90 patients were enrolled. Ten patients, (4 patients from LMA group and 6 from NPA group) were excluded from the study either due to change of the technique to rigid bronchoscopy (e.g. accicentally discovered foreign body) or complications that cancelled the procedure (e.g. severe larygospasm or bronchospasm with Persistant hypoxemia that needed muscle relaxation and mechanical ventilation).
The Demographic data showed no statistically significant differences in patient characteristics regarding age, sex, weight, height and ASA classification (Table 1).
| Variables measured | Groups | |||
|---|---|---|---|---|
|
LMA (N=45) |
NPA (N=45) |
T-test | ||
| t | P-value | |||
| Age (years) | 6.5 ± 2.5 | 7.2 ± 2.3 | 1.459 | 0.148 |
| Sex F/M | 20/25 | 22/23 | 0.179 | 0.637 |
| Weight (kg) | 23.7 ± 3.4 | 24.1 ± 2.4 | 0.618 | 0.538 |
| Height (cm) | 119.8 ± 3.5 | 121 ± 4.3 | 1.452 | 0.150 |
| ASA I/II | 38/7 | 40/5 | 0.385 | 0.535 |
| HR (beats/min) | 115.2 ± 7.5 | 117.3 ± 8.5 | 1.229 | 0.222 |
| SBP (mmHg) | 90.2 ± 5.2 | 92.5 ± 4.4 | 2.183 | 0.031* |
| DBP (mmHg) | 50.4 ± 4.2 | 52.1 ± 4.5 | 1.868 | 0.065 |
Regarding the hemodynamic monitoring, there was no significant difference between the two groups in the heart rate and diastolic blood pressure, however, the systolic blood pressure was lower with significant difference in LMA group than in NPA group (Table 1)
On comparing both groups considering desaturation (SpO2 < 90%) during procedure and the total number of patients had desaturation the results showed that the number of patients having desaturation episodes was more in group LMA than group NPA with highly significant difference (p-value 0.005). Also, SpO2 dropped in LMA group to lower values more than NPA group with highly significant difference (p-value < 0.001) (Table 2).
In addition, we recorded the duration of the procedure from induction till recovery between both groups. The total time of procedure was significantly less in NPA group than in LMA group (p-value < 0.001). Also, the total consumption of propofol was higher in LMA group than in NPA group with statistically highly significant difference (p-value < 0.001) (Fig. 1, Table 3).
| Variables Measured | Groups | |||
|---|---|---|---|---|
|
LMA (N=45) |
NPA (N=45) |
T-test | ||
| t | P-Value | |||
| Baseline Spo2% | 96.94 ± 2.57 | 97.18 ± 2.64 | 0.437 | 0.663 |
| Lowest Spo2% | 86.38 ± 3.53 | 91.72 ± 3.98 | 6.734 | <0.001** |
| Change in Spo2% | 11.11% | 4.44% | ||
| Desaturation Patients n (%) | 19(42.22%) | 7(15.56%) | 7.788 | 0.005* |
| Duration of Procedure | Groups | |||||
|---|---|---|---|---|---|---|
| LMA (N=45) |
NPA (N=45) |
T-test | ||||
| N | % | N | % | T | P-value | |
| 15 min | 8 | 17.8 | 19 | 42.2 | ||
| 20 min | 13 | 28.8 | 15 | 33.3 | ||
| 25 min | 12 | 26.6 | 7 | 15.5 | ||
| 30 min | 8 | 17.7 | 4 | 8.8 | ||
| 35 min | 4 | 8.9 | 0 | 0.0 | ||
| Total duration (Mean± SD)min | 25.29 ± 3.64 | 18.53 ± 3.28 | 9.255 | <0.001** | ||
| Total propofol dose mg | 1505.14 ± 245.78 | 420.17 ± 75.38 | 28.311 | <0.001** | ||
Furthermore, we studied the effect of ventilation on the change in PaCO2 during the procedure by measuring a baseline PaCO2 and another sample at the end of the procedure, and it was observed that the change was higher in LMA group than in NPA group, but no statistically significant difference was found between both groups (p-value 0.086) (Table 4)
| Intraoperative data | Groups | |||
|---|---|---|---|---|
|
LMA (N=45) |
NPA (N=45) |
T-test | ||
| Mean ± SD | Mean ± SD | t | P-value | |
| 1st paCO2 | 31.52 ± 2.34 | 32.31 ± 2.49 | 1.551 | 0.124 |
| 2nd paCO2 | 50.24 ± 4.85 | 48.39 ± 5.27 | 1.733 | 0.086 |
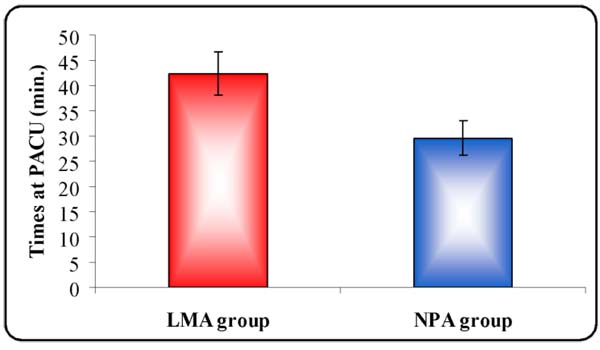
As the time passed at the PACU to detect the effect of both techniques on the recovery time, the results showed prolonged recovery time in LMA group than in NPA group with statistically significant difference between both groups (p-value < 0.001) (Table 5).
| Times at PACU | Groups | |||||
|---|---|---|---|---|---|---|
| LMA (N=45) |
NPA (N=45) |
T-test | ||||
| N | % | N | % | T | P-value | |
| 20 min | 0 | 0.0 | 5 | 11.1 | ||
| 30 min | 14 | 31.1 | 37 | 82.2 | ||
| 40 min | 15 | 33.3 | 3 | 6.7 | ||
| 50 min | 10 | 22.2 | 0 | 0.0 | ||
| 60 min | 6 | 13.3 | 0 | 0.0 | ||
| Total time (Mean± SD) min | 41.60 ± 4.36 | 30.25 ± 3.15 | 14.155 | <0.001** | ||
4. DISCUSSION
This present study compared the use of laryngeal mask airway versus nasopharyngeal airway as alternative techniques for ventilating children undergoing diagnostic flexible fibreoptic bronchoscopy. The use of NPA resulted in significant reduction in hypoxemia and desaturation episodes together with shorter procedure and recovery time using lesser doses of propofol.
One of the alternative techniques of airway management in this field is spontaneous breathing of patients using supraglottic devices. They observed to be simple and feasible and associated with less hemodynamic and oxygenation instability [5-9]. The current study also showed no clinical relevant changes in heart rate values. However, we found that systolic blood pressure dropped more in LMA group than in NPA group, but without clinical significance, this might be related to the larger doses of propofol used in LMA group.
Previous authors have used widely variable reductions in SpO2 to define desaturation leading to significant heterogeneity. For instance, Nussbaum [10] defined desaturation as a drop in SpO2 to 65%-80%, Rodrıguez et al. [11] defined it as a drop in SpO2 of 10% or more below the baseline. In the present study, we considered a decrease in spO2 ≤ 90% as a desaturation episode. The studies of Schnapf [12] and Peng et al. [13] in oxygen desaturation during pediatric fibreoptic bronchoscopy have related the desaturation to the age and the skills of the operator. However, in the current study, since we had a single operator, we related it to the technique, we found that due to unshared airway with the same operator the NPA group had better oxygenation and significantly lesser frequency of desaturation than LMA SpO2 group (15.56% and 41.7%, respectively) also lowest SpO2 in NPA and LMA(92.63% and 3.05 & 86.41% ± 3.81, respectively). Furthermore, the bronchoscopy time was longer in group LMA than in group NPA with highly significant difference (10 patients in group LMA and only 2 patients in group NPA lasted more than 30 minutes). The longer duration is assumed to be due to the repeated episodes of deoxygenation during the procedure.
It should be noted that we did not use a bronchoscopy adapter to the LMA which could be a limitation to our study since it could have resulted to an increase in episodes of desaturation on LMA group, however, previous studies that used this special bronchoscopy adaptor didn’t determine its value regarding the frequency of desaturation or length of the procedure.
As a result of the lengthy procedure time in LMA group, the study showed that the overall propofol consumption during the procedure was higher in LMA group than in NPA group with highly significant difference (p-value < 0.001). Yarmus et al. [14] proved that the use of LMA technique requires more depth of anesthesia. Grendelmeier et al. [15] also found that longer bronchoscopy time has higher requirements of propofol and it is safe whether used as bolus or as continuous infusion.
In order to evaluate the impact of using both techniques on hypoventilation that might occur during the procedure, we measured PaCO2 at two time intervals: the 1st post-induction; and the second just before recovery for each patient. The difference between the two samples was calculated. The increase in PaCO2 was higher in group LMA than in group NPA with no significant difference (p-value < 0.086).
Diagnostic flexible fibreoptic bronchoscopy is considered a day case procedure, we used modified aldret’s score with score ≥ 9 to discharge patient from PACU after recording the recovery time inside the PACU, the LMA group had longer recovery time in the PACU than NPA group (41.60 min ±4.36 & 30.25 min ±3.15, respectively). Also, 31 patients in LMA group stayed more than 30 minutes in the PACU, while only 3 in NPA group, this could be attributed to longer procedure time and larger doses of propofol given to deepen anesthesia in LMA group.
CONCLUSION
In conclusion, the use of NPA as supraglottic ventilating device for ventilating children undergoing diagnostic flexible fibreoptic bronchoscopy is considered a good alternative for shortening the bronchoscopy time with less frequency of desaturation and better recovery compared with LMA ventilation technique.
ETHICS APPROVAL AND CONSENT TO PARTICIPATE
The participants were enrolled from June 2016 to March 2017 after the approval of the Ethical Medical Committee and obtained a written informed consent from their parents or guardians.
HUMAN AND ANIMAL RIGHTS
No animals were used. All clinical investigations were conducted according to the Declaration of Helsinki principles.
CONSENT FOR PUBLICATION
Not applicable.
CONFLICT OF INTEREST
The authors declare no conflict of interest, financial or otherwise.
ACKNOWLEDGEMENTS
Declared none.


