All published articles of this journal are available on ScienceDirect.
Effect of Pentoxifylline on Organ Dysfunction and Mortality in Severe Sepsis
Abstract
Background:
Sepsis and infection are among the leading causes of death world-wide. The annual burden of sepsis in high-income countries is rising with a mortality rate of 40% and 90% of the worldwide deaths from pneumonia, meningitis or other infections occur in less developed countries. This study was performed to evaluate the therapeutic efficacy of pentoxifylline as an adjuvant therapy in septic patients and its effect on multiple organ dysfunction and mortality in septic patients.
Methods:
This randomized, double-blinded prospective study was conducted from October 2017 to November 2018, which included a total sample size of 52 cases of septic patients. Organ dysfunction was used as a primary outcome with proposed large effect size ((0.8) and alfa =0.05 and power=0.80, so, 26 cases were needed in each group). Secondary outcomes were inflammatory markers C-Reactive Protein (CRP) and pro-calcitonin, duration of hospital stay, need for hemodialysis, need for vasopressor & inotropes, need for mechanical ventilation and 28 days survival.
Results:
Fifty-two patients with sepsis were divided in 1: 1 ratio to receive pentoxifylline or not. The average age of the included patients was almost 53 years, chest disorders were the main cause of sepsis in both groups. There were no statistically significant differences between both groups in terms of Sequential Organ Failure Assessment (SOFA) score, lactate level, CRP level and pro-calcitonin level. As regards secondary outcomes, there were no statistically significant differences between study’s groups in terms of length of hospital stay (p =0.707), need for hemodialysis (p =0.541), need for vasopressor & inotropes (p =0.249), need for mechanical ventilation (p =0.703), and 28 days survival (p =0.5).
Conclusion:
We concluded that pentoxifylline as an adjuvant therapy in septic patients had no significant influence on multiple organ dysfunction and mortality.
1. INTRODUCTION
Sepsis and infection are among the leading causes of death world-wide. The annual burden of sepsis in high income countries is rising with a mortality of 40%. Despite these figures from industrialized countries, the largest part of the global sepsis burden occurs in middle and low- income countries, 90% of the worldwide deaths from pneumonia, meningitis or other infections occur in less developed countries [1].
Severe sepsis is defined as sepsis associated with organ dysfunction, hypoperfusion, or hypotension. Perfusion abnormalities may include but are not limited to, lactic acidosis, oliguria, or alteration in mental status [2]. In 2016, the surviving sepsis campaign defined sepsis as a life-threatening organ dysfunction caused by the dysregulated host response to an infection [3].
In septic patients, Tumor Necrosis Factor-alfa (TNF-α) is the first pro-inflammatory cytokine that is released, followed by interleukin (IL)-1, IL-6, and IL-8. TNF-α and IL-1 are the most important pro-inflammatory cytokines; they are biologically closely related, act synergistically, and are largely responsible for the clinical manifestation of sepsis [4].
Pentoxifylline (PTX), (1-[5-oxohexyl]-3, 7-dimethylxanthine), a methylxanthine derivative and non-specific phosphodiesterase inhibitor, among its other actions, inhibits the production of TNF-α, preserves microvascular blood flow, prevents circulatory failure and intestinal vasoconstriction and has beneficial effects on endothelial cell function and coagulation in sepsis [5].
PTX enhances anti-inflammatory activity and decreases mortality in acute endotoxemia and may be an important adjunct to therapies aiming to modulate the inflammatory response in sepsis [5]. This study was conducted to evaluate the therapeutic efficacy of pentoxifylline as an adjuvant therapy in severe sepsis and its effect on multiple organ dysfunction and mortality in septic patients.
2. METHODS
This randomized, double blinded prospective study was conducted between October 2017 to November 2018 at Ain Shams University Hospitals' Intensive Care Units and Maadi Military Hospital on patients with severe sepsis according to the definitions of Sepsis Surviving Campaign (SSC) 2016 [3]. Total sample size of 52 cases organ dysfunction using SOFA score was used as a primary outcome with proposed large effect size ((0.8) and alfa=0.05 and power=0.80, so, 26 cases were needed in each group). Secondary outcomes were inflammatory markers (CRP and pro-calcitonin), duration of hospital stay, need for hemodialysis, need for vasopressor & inotropes, need for mechanical ventilation and 28 days survival.
2.1. Selection Criteria of the Studied Groups
2.1.1. Inclusion Criteria
- 1- Adult patients age ≥18 years.
- 2- Patients with severe sepsis. The diagnosis of severe sepsis was established according to the definitions of SSC [3].
- 3- Sepsis was due to either nosocomial pneumonia or pelvic-abdominal sepsis.
2.1.2. Exclusion Criteria
(1) Late septic shock at presentation with multiple organ failure.
(2) APACHE II score on admission >25.
(3) Preexisting liver cirrhosis.
(4) Preexisting end stage renal disease
(5) Pregnancy.
(6) History of allergy or intolerance to Pentoxifylline.
(7) Patient with malignancies
(8) Uncontrolled hemorrhage
(9) Burn
(10) Previous steroid therapy
(11) Death within 24 hours of ICU admission
Patients who were diagnosed as having severe sepsis due to either nosocomial pneumonia or pelvi-abdominal sepsis; and did not meet any of the exclusion criteria were prospectively included in the study then randomly divided to either receiving conventional sepsis therapy alone according to guidelines or to receive conventional sepsis therapy in addition to pentoxifylline 1 mg/kg/hour intravenous maximum 1800 mg/day during 28 days or until they were discharged from the intensive care unit or died.
2.2. Patients with Severe Sepsis were Subjected to the Following
2.2.1. Clinical Evaluation
History and physical examination with special emphasis on vital signs (Blood pressure, pulse, Temperature and Respiratory Rate) and Glasgow Coma Scale were continuously evaluated.
2.2.2. Routine Laboratory Investigations
- CBC (complete blood count)
- Coagulation profile: PT, INR and PTT.
- ABGs (Arterial Blood Gases).
- Central Venous Oxygen Saturation.
- Liver Function Tests: Alanine aminotransferase (ALT), Aspartate aminotransferase (AST), Total bilirubin (TBL) and albumin.
- Kidney Function Tests: urea, and serum creatinine.
These routine tests were conducted daily.
On day 1, 3, 7, 10 and 14.
2.2.3. Microbiological Studies
Including cultures (sputum, blood, urine or biological fluid according to clinical suspicion) on day 1.
2.2.4. Imaging Studies
Required to Identify the Source of Sepsis e.g. (pelvi-abdominal CT, Ultrasound and Chest x-ray).
2.2.5. Clinical Data
The following data were evaluated up to a maximum follow up period of 28 days of ICU stay.
- Length of hospital stay.
- Need for and duration of Mechanical Ventilation (MV).
- Need for and duration of vassopresor and inotropic support.
- Need for haemodialysis.
2.2.5.1. Final Outcome Survivors
A) Patients recovered and discharged from Intensive Care Unit (ICU).
B) Patients still morbid and stayed in ICU for more than 28 days.
2.2.5.2. Non-Survivors
Death before the Completion of the 28 Days of the Study Period
2.2.6. Application of APACHE II and SOFA Scoring Systems
APACHE II score was evaluated on study day 1; while SOFA score was evaluated on study day 1 and serially every day until ICU discharge or death or up to 28 days.
2.3. Statistical Analysis and Sample Size
Data entry, processing, and statistical analysis were carried out using MedCalc version 15.8. Frequency tables with percentages were used for categorical variables and descriptive statistics (mean ± standard deviation or median with interquartile range) were used for numerical variables. Tests of significance (Chi-square, student’s t-test, or Mann Whitney’s test) were used according to the normality of the data. A P-values of less than 0.05 was considered statistically significant. Total sample size of 52 cases (organ dysfunction using SOFA score was used as a primary outcome with proposed large effect size (0.8) and alfa=0.05 and power=0.80, so, 26 cases were needed in each group
3. RESULTS
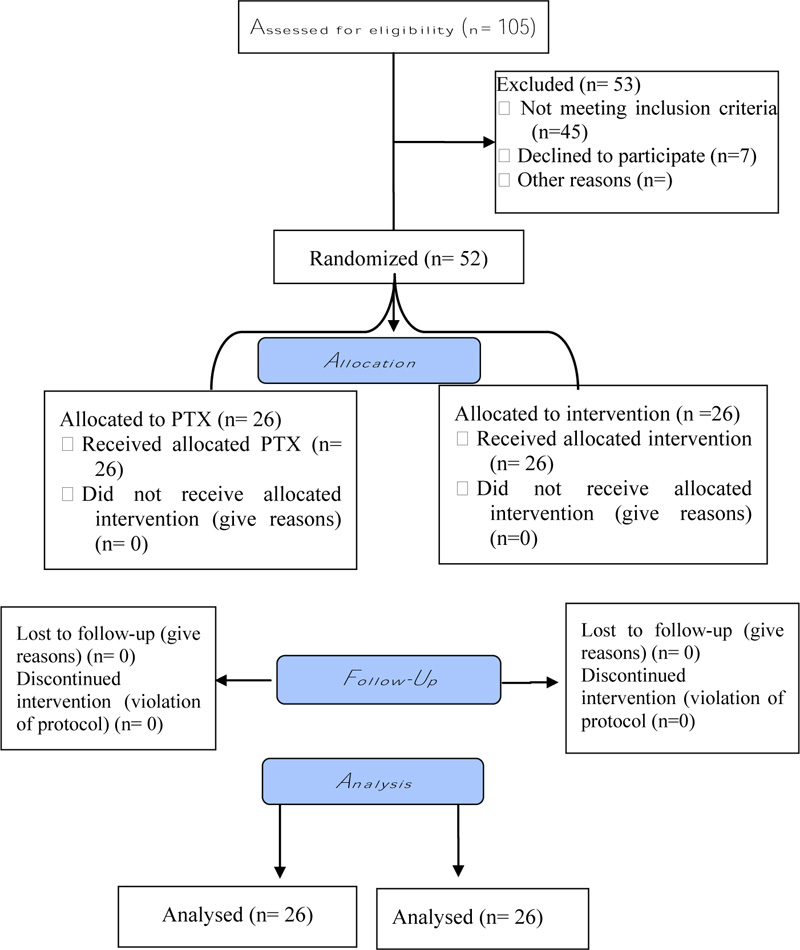
This randomized, double-blinded prospective study was conducted from October 2017 to November 2018, 105 septic patients were assessed for eligibility, but only 52 patients were included in the study (Fig. 1). The average age of the included patients was almost 53 years, chest disorders were the main cause of sepsis in both groups (Table 1). Considering the baseline clinical parameters, there were no statistically significant differences between both groups in terms of SOFA score (p =0.496), APACHE II score (p =0.26), lactate level (p =0.235), CRP level (p =0.503), and pro-calcitonin level (p =0.698) (Table 2). On day 3, there were no statistically significant differences between both groups in terms of SOFA score (p =0.629), lactate level (p =0.209), CRP level (p =0.934), and pro-calcitonin level (p =0.502) (Table 3). Similarly, day 7 showed no statistically significant differences between both groups in terms of SOFA score (p =0.58), lactate level (p =0.303), CRP level (p =0.253), and pro-calcitonin level (p =0.466) (Table 4). On day 10, there were no statistically significant differences between both groups in terms of SOFA score (p =0.316), lactate level (p =0.39), CRP level (p =0.624), and pro-calcitonin level (p =0.209) (Table 5). In terms of the primary outcome on day 14, SOFA score was numerically lower in pentoxifylline group than the control group, however, the difference was not statistically significant (p =0.655). Similarly, there was no significant difference between both groups in terms of lactate level (p =0.574), CRP level (p =0.740), and pro-calcitonin level (p =0.707) (Table 6). Regarding secondary outcomes, there was no statistically significant difference between studied groups in terms of length of hospital stay (p =0.707), need for hemodialysis (p =0.541), need for vasopressor & inotropic support (p =0.249), need for mechanical ventilation (p =0.703), and 28 days survival (p =0.5) (Table 7).
4. DISCUSSION
The word sepsis was used as early as the time of the ancient Greeks to describe decomposition or putrefaction [6]. In 2001, an attempt was made to revisit the systemic inflammatory response syndrome criteria, but the resultant list of signs and symptoms of sepsis was too long to be widely accepted, and the systemic inflammatory response syndrome criteria, however inadequate, continued to be used [7].
In 2016, the Society of Critical Care Medicine (SCCM) and the European Society of Intensive Care Medicine propose that sepsis be regarded as the presence of life-threatening organ dysfunction, quantified by an increase in SOFA of at least 2 for the organ in question, which occurs as the result of a dysregulated host response to an infection [3].
In septic patients, TNF-α is the first pro-inflammatory cytokine that is released, followed by IL-1, IL-6, and IL-8. PTX enhances anti-inflammatory activity and decreases mortality in acute endotoxemia. PTX may be an important adjunct to therapies aiming to modulate the inflammatory response in sepsis [5].
We conducted this study to assess the therapeutic efficiency of PTX as adjuvant therapy in the treatment of severe sepsis and its effect on multiple organ dysfunction and mortality in the Intensive Care Unit (ICU).
Our results showed that the SOFA score was numerically lower in the PTX group than the control group, however, the difference was not statistically significant (mean (SD)= 7.48 (7.6) in PTX versus 8.39 (7.07) in control, p=0.655). This finding came in contrast with a previous double-blind, placebo-controlled study that randomized 51 surgical patients with severe sepsis to receive PTX continuously (27 patients) or saline infusion as placebo (24 patients). Patients received PTX (1 mg/kg of body weight per hour; maximum, 1800 mg/d) for 28 days or until they were discharged from the intensive care unit or died. The results showed that the multiple organ dysfunction score was significantly reduced in the PTX group than the placebo group [8]. Difference in the calculation of organ failure, co-interventions, and influences that impact organ failure between this and the previous study may justify this contradiction.
Regarding the lactate level, our results showed no significant difference between the PTX group and the control group (mean (SD)= 6.56 (4.5) in PTX versus 6.87(3.8) in control, p= 0.58). Previous studies have reported the use of lactate as a marker for diagnosis, prognosis, and treatment of tissue hypoxia in shock. A patient with severe sepsis with significant hypoperfusion (lactate > 4 mmol/l) is considered to be in shock even without the necessary hypotension criteria. Therefore, there is enough evidence to state that normotensive patients with severe sepsis and significant lactic acidosis, should receive early antibiotics, hemodynamic monitoring and adequate resuscitation [9].
Our results showed that the PTX group and the control group were comparable in terms of CRP level (mean (SD) = 81.32 (74) in PTX versus 85.57 (64.9) in control, p= 0.740). This is in agreement with a prospective, double-blind, controlled study, which enrolled 104 new-borns with suspicion of sepsis. The patients were divided into four groups according to treatment protocol: Group 1 = placebo, Group 2 = PTX, Group 3 = IgM-enriched IVIG, and Group 4 = PTX + IgM-enriched IVIG. Blood samples were taken for C-reactive protein, interleukin-6, neutrophil CD64 expression, and TNF-α measurements immediately before treatment (1st day), and measurements were repeated on the 2nd and 4th days of the therapy. The results showed that there was no significant difference among compared groups regarding CPR level [10].
However, this finding is in contrast to the study by Shabaan et al. [11], which included 120 preterm infants with late-onset sepsis, who were randomly assigned to receive either intravenous PTX 5 mg/kg/hr for 6 hours on 6 successive days or placebo. The results showed that PTX was associated with a significant reduction in CRP than placebo. Shabaan et al. used PTX 5 mg and enrolled preterm infants; therefore, the differences in the doses of PTX in addition to the differences in study populations may justify this contrary.
Regarding procalcitonin level, our analysis showed that there was no significant difference between PTX and control (mean (SD) = 7.53 (7.3) in PTX versus 8.14 (5.92) in control, p=0.71). Procalcitonin is one of the most useful markers of systemic bacterial infection [12]. Compared to all other currently available sepsis markers, procalcitonin is valuable in the differentiation between infectious and non-infectious systemic inflammation in low acuity patients [12, 13].
| Variables | Pentoxifylline Group (N =26) | Control Group (N=26) | P-value | ||
|---|---|---|---|---|---|
| No | % | No | % | ||
|
Age in years 1. Mean (SD) |
53.42 (10.57) | 53.77 (9.54) | 0.902 | ||
|
Weight in Kg 1. Mean (SD) |
84.50 (11.25) | 83.65 (10.54) | 0.78 | ||
| Gender | - | - | - | - | - |
| 1. Male | 17 | 65.4 | 18 | 69.2 | 0.99 |
| 2. Female | 9 | 34.6 | 8 | 30.8 | - |
| Causes of Sepsis | - | - | - | - | - |
| 1. ABDOMEN | 5 | 19.2 | 7 | 26.9 | - |
| 2. CHEST | 16 | 61.5 | 15 | 57.7 | 0.47 |
| 3. UTI | 5 | 19.2 | 4 | 15.4 | - |
| Variable | Pentoxifylline Group (N =26) | Control Group (N=26) | Mann-Whitney Test | P-value |
|---|---|---|---|---|
| SOFA score | - | - | - | - |
| - Median (IQR) | 8 (6.75 -12) | 9 (7 -12.25) | - | 0.496 |
| APACHE II score | - | - | - | - |
| - Median (IQR) | 13 (11-14) | 12 (11-14) | - | 0.26 |
| Lactate at baseline (mmol/L) | - | - | 276.000 | 0.235 |
| - Mean (SD) | 8.77 (2.9) | 9.62 (2.9) | ||
| CRP (mg/dL) | - | - | 298.000 | 0.503 |
| - Mean (SD) | 109 (40.3) | 108.5 (43.37) | ||
| Pro-calcitonin (ng/ml) | - | - | 317.000 | 0.698 |
| - Mean (SD) | 12.81 (2.62) | 12.92 (2.62) |
| Variable |
Pentoxifylline Group (N =26) |
Control Group (N=26) |
Mann-Whitney Test | P-value |
|---|---|---|---|---|
| SOFA score | - | - | - | - |
| - Median (IQR) | 10 (5 -11.25) | 9.5 (6.75 -12) | - | 0.626 |
| Lactate (mmol/L) | - | - | 270.000 | 0.209 |
| - Mean (SD) | 8.65 (2.74) | 9.58 (2.87) | ||
| CRP (mg/dL) | - | - | 333.500 | 0.934 |
| - Mean (SD) | 120.08 (45.7) | 121.38 (45.4) | ||
| Pro-calcitonin (ng/ml) | - | - | 301.500 | 0.502 |
| - Mean (SD) | 10.92 (3.82) | 11.42 (3.22) |
| Variable |
Pentoxifylline Group (N =26) |
Control Group (N=26) |
Mann-Whitney Test | P-value |
|---|---|---|---|---|
| SOFA score | - | - | - | - |
| - Median (IQR) | 8 (4.75 – 11.25) | 9 (5 -14.25) | - | 0.58 |
| Lactate (mmol/L) | - | - | 282.000 | 0.303 |
| - Mean (SD) | 8.42 (3.28) | 9.15 (3.33) | ||
| CRP (mg/dL) | - | - | 275.500 | 0.253 |
| - Mean (SD) | 104.46 (58.8) | 118.42 (58.18) | ||
| Pro-calcitonin (ng/ml) | - | - | 296.500 | 0.446 |
| - Mean (SD) | 9.81 (5.16) | 10.65 (4.4) |
| Variable |
Pentoxifylline Group (N =26) |
Control Group (N=26) |
Mann-Whitney Test | P-value |
|---|---|---|---|---|
| SOFA score | - | - | - | - |
| - Median (IQR) | 5.5 (2.75 – 9.75) | 7 (3.5 – 16) | - | 0.316 |
| Lactate (mmol/L) | - | - | 280.000 | 0.39 |
| - Mean (SD) | 7.54 (4.16) | 8.24 (3.53) | ||
| CRP (mg/dL) | - | - | 299.000 | 0.624 |
| - Mean (SD) | 92.5 (64.8) | 102.64 (66.43) | ||
| Pro-calcitonin (ng/ml) | - | - | 269.000 | 0.209 |
| - Mean (SD) | 8.425 (6.34) | 9.76 (5.06) |
| Variable | Pentoxifylline | Control | Mann-Whitney Test | P-value |
|---|---|---|---|---|
| SOFA score | - | - | - | - |
| - Median (IQR) | 5 (2 -13.5) | 5 (3 -16) | - | 0.655 |
| Lactate (mmol/L) | - | - | 260.500 | 0.574 |
| - Mean (SD) | 6.56 (4.5) | 6.87 (3.8) | ||
| CRP (mg/dL) | - | - | 271.500 | 0.740 |
| - Mean (SD) | 81.32 (74) | 85.57 (64.9) | ||
| Pro-calcitonin (ng/ml) | - | - | 317.500 | 0.707 |
| - Mean (SD) | 7.532 (7.3) | 8.1391 (5.92) |
| Variables |
Pentoxifylline Group (N =26) |
Control Group (N=26) |
P-value | ||
|---|---|---|---|---|---|
| No | % | No | % | - | |
| Length of hospital Stay | - | - | - | ||
| - Mean (SD) | 21.31 (5.95) | 22.92 (9.49) | 0.707 | ||
| Need for hemodialysis | - | - | - | - | - |
| - Yes | 6 | 23.1 | 9 | 34.6 | 0.541 |
| - No | 20 | 76.9 | 17 | 65.4 | - |
| Need for Vasopressor & Inotropic support | - | - | - | - | - |
| - Yes | 21 | 80.8 | 23 | 88.5 | 0.249 |
| - No | 5 | 19.2 | 3 | 11.5 | - |
| Duration of Vasopressor & Inotropic, days | - | - | 0.15 | ||
| - Mean (SD) | 7.8 (1.02) | 7.4 (0.98) | |||
| Need for mechanical ventilation | - | - | - | ||
| - Yes | 14 | 53.8 | 16 | 61.5 | 0.703 |
| - No | 12 | 46.2 | 10 | 28.5 | - |
| Duration of mechanical ventilation | - | - | 0.19 | ||
| - Mean (SD) | 7.2 (1.1) | 6.8 (1.09) | |||
| Survived | - | - | - | ||
| - Yes | 20 | 76.9 | 19 | 73.1 | 0.5 |
| - No | 6 | 23.1 | 7 | 26.9 | - |
Considering secondary outcomes, there were no statistically significant differences between study groups in terms of length of ICU stay (mean (SD)= 21.31 (5.95) in PTX versus 22.92 (9.49) in control, p =0.707), need for HD (N (%)= 6 (23.1%) in PTX versus 9 (34.6%) in control, p =0.541), need for vasopressor and inotropic (21 (80.8%) in PTX versus 23 (88.5%) in control, p =0.249), need for MV (14 (53.8%) in PTX versus 16 (61.5%) in control, p =0.703). In agreement with our results, Akdag et al. [10] did not find a significant effect of PTX on the length of hospital stay compared to placebo (median (range) in days= 28 (5-246) in PTX versus 27 (1-168) in placebo).
On the other hand, Shabaan et al. [11] found that the length of hospital stay was significantly lower in the PTX group than the placebo group (31.3 (12.2) in PTX versus 38.3 (12.3) in placebo, p=0.04). Furthermore, patients in the PTX group had less need for vasopressors support than those in the placebo group. The variations in the PTX doses and study populations may justify this contrary.
Regarding mortality rate, our results showed no significant difference between PTX and control (6 (23.1%) in PTX versus 7 (26.9%) in control, p= 0.5). Our results accord with the findings of Staubach et al. [8], who reported that PTX and placebo were comparable in terms of 28-day mortality (8/27 (30%) in PTX versus 8/24 (33%) in placebo). Moreover, the results by Shabaan et al. [11] did not favour PTX over control in mortality rate (6 (10%) in PTX versus (10 (16.5%) in placebo, p= 0.44). In addition, Akdag et al. [10]. found no significant difference between PTX and placebo regarding the mortality rate (5 (9.8%) in PTX versus 2 (3.9%) in placebo.
CONCLUSION
We concluded that PTX as adjuvant therapy in severe sepsis had no significant influence on the SOFA score, lactate level, CRP level, and pro-calcitonin level compared to control. Moreover, there were no statistically significant differences in terms of length of hospital stay, need for hemodialysis, need for vasopressor and inotropic, need for MV, and mortality rate. Further large clinical trials are recommended to assess the effectiveness of PTX, especially with regards to organ failure, survival, and dose dependency.
AUTHOR CONTRIBUTIONS
Haytham M. Ibrahim has full access to all the data in the study and takes responsibility for the integrity of the data. Bahaa El Deen E. Hasan, Hanaa A. El Gendy and Amr S. Abd El Kawe designed and conceptualized the study. Haytham M. Ibrahim, Bahaa El Deen E. Hasan, Hanaa A. El Gendy and Amr S. Abd El Kawe acquired the data. Analysis and interpretation of data: Bahaa El Deen E. Hasan, Hanaa A. El Gendy, Amr S. Abd El Kawe . Haytham M. Ibrahim drafted the manuscript. Bahaa El Deen E. Hasan, Hanaa A. El Gendy and Amr S. Abd El Kawe critically revised the manuscript for intellectual content.
ETHICS APPROVAL AND CONSENT TO PARTICIPATE
The Faculty of Medicine Research Ethics committee approval was taken (FWA 000017585).
HUMAN AND ANIMAL RIGHTS
Not applicable.
CONSENT FOR PUBLICATION
Written consent was taken from the patients or the next of kins.
STANDARD OF REPORTING
CONSORT guidelines and methodology were followed.
FUNDING
None.
CONFLICTS OF INTEREST
The authors declare no conflict of interest, financial or otherwise.
ACKNOWLEDGEMENTS
We would like to thank all our colleagues at the Ain Shams University Hospitals' Intensive Care Units and Maadi Military Hospital who performed extensive data entry.


