All published articles of this journal are available on ScienceDirect.
Repeated Thoracic Paravertebral Blocking to Alleviate Pain Symptoms in 66-years-old Man with Post-herpetic Neuralgia: A Case Report
Abstract
Introduction
Post-herpetic Neuralgia (PHN) is a neuropathic pain syndrome resulting from the sequelae of Herpes Zoster (HZ).
Case Report
Therefore, this study aimed to report a case of a 66-year-old male who presented with chronic pain characterized by a burning sensation in the right chest region, specifically at the areola level. The patient had been experiencing these symptoms for a year, which progressed to the severe stage over the past few months. To mitigate pain, a Thoracic Paravertebral Block (TPVB) procedure was proposed and conducted 3 times, with a solution containing levobupivacaine 0.25% and dexamethasone 10 mg in 5 ml.
Conclusion
The procedure was replicated three times. After two weeks, the pain had almost subsided, showing less need for further analgesia.
1. INTRODUCTION
Post-herpetic Neuralgia (PHN) is a neuropathic pain syndrome resulting from the sequelae of Herpes Zoster (HZ). It originates from Varicella Zoster Virus (VZV) reactivation following decades of latent phase in an individual body. Pain experienced significantly impacts daily life activities and overall quality of life [1, 2]. Furthermore, it often persists as a feature following HZ in at least 5%-20% of cases, leaving a significant portion of the population contending with a chronic condition that requires treatment. This prevalence is substantial as the source of PHN or evidence of VZV infection can typically be identified in the adult population, estimated to occur in more than 99% of individuals throughout their lifetime [3, 4].
Several analgesic classes have been described to address neuropathic pain, with tricyclic antidepressants (such as nortriptyline and desipramine) and calcium channel α2-δ ligand agents (such as gabapentin and pregabalin) considered first-line standards for PHN. Opioid class agents (oxycodone, morphine, methadone, tramadol, etcf.) are the second-line approach in cases where PHN symptoms are refractory during the treatment course [1, 2, 5]. However, the use of more potent medications comes with considerable adverse reactions, ranging from dizziness to hypotensive events, thereby creating additional challenges. On the other hand, nerve block techniques, such as epidural and intrathecal methods, offer a more direct intervention to the affected nerve fibers. Among the available approaches, significant interest is given to TPVB, as it has been extensively studied for alleviating neuropathic symptoms in the thoracal region [6-8].
The relevance of the TPVB procedure is supported by accompanying Ultrasonography (USG) imaging. Incorporating the procedure in clinical practice and establishing a current state-of-art method depend on two major variables, namely the patient and the operator [7, 8]. While selecting a suitable individual presents a challenge, fully embracing the invasive TPVB to alleviate pain relies on the operator, a facet explored in this study. This work aimed to elaborate on the status of the TPVB procedure in Indonesia for managing PHN. The approach was proposed on a broader scale to effectively handle pain and reduce drug consumption over the long term.
2. CASE PRESENTATION
A 66-year-old male presented with symptoms of pain in the right chest for approximately a year, which subsequently intensified over the past few months. The pain was persistently endured, but became severe during the act of wearing clothes. Furthermore, it initially coincided with the eruption of several vesicles on the right chest area at the areola level, extending from the anterior to the posterior side of the body. The patient described the pain as pulsating and a “burning-like” sensation with a reported severity of 7-8 out of 10 according to VAS measurement during history taking. Additionally, a significant bothering itchy sensation was experienced on the lesions. The vesicles were small (1.0-2.0 mm) and multiple, diagnosed as HZ without prior vaccination history. Despite the unclear administration of anti-viral agents, the patient received a series of analgetic drugs, which proved to be ineffective, offering only mild symptom attenuation. Finally, prodromal symptoms were observed to be positive.
After several days, the skin lesions in the affected region diminished, but the pain persisted. Despite the reduced severity, the pain remained a significant concern. Touching the post-vesicle area generated an “electricity-like” sensation, leading to a severity level of 9-10/10, which was described by the patient as a worse experience. Consequently, the sleep sessions of the patient were highly troubled and the emotions deteriorated daily, manifesting in the form of difficulty in concentrating, high temper, and moodiness.
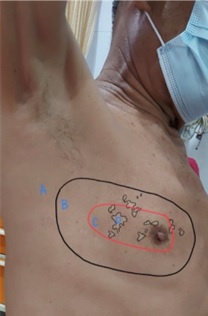
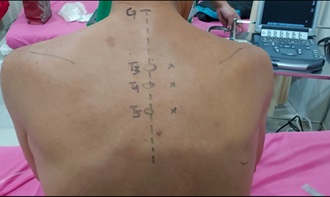
During the physical examination, vital signs were normal. Assessment of the localized area of the chest showed several hypo-pigmented lesions around the right areola without any redness and edema, as presented in Fig. (1). No sensory deficits were recorded during previous admission to a neurologist. The routine hematologic checkup was within normal range, leading to the diagnosis of Post-herpetic Neuralgia (PHN). Furthermore, TPVB was performed 3 times at the Th3 to Th5 level of the vertebra after providing an explanation and obtaining informed consent. Based on Ultrasonography (USG) procedures, levobupivacaine 0.25% (Levica®) and dexamethasone 10 mg in 5 ml solution were injected at each vertebra level after being induced by stimuflex® ultra 360® needles in the plane to the respective paravertebral spaces (Fig. 2).
The patient was observed for ±1 hour to identify any adverse reactions affecting vital sign status, occurrence of motoric blockage event, or drug-specific allergic eruptions. The condition remained stable as the procedure was repeated on the 3rd and 6th day post-first TPVB plus oral medication administration, including pregabalin (2 x 75 mg), amitriptyline (1 x 12.5 mg), methylcobalamin (1 x 1), and laxansia. Respectively, pain was instantly reduced to 2-3 in 1st procedure, as well as 1-2 in the 2nd and 3rd on VAS. Consequently, all accompanying issues, such as lowered appetite and disturbed sleep, showed significant improvement. Approximately 2 weeks post-first TPVB, the patient ceased consuming oral drugs, as pain level reduced to 1 out of 10. Finally, the patient reported a return to normal activities without any significant disturbance.
Ethical approval was received from the health research ethics committee of the Faculty of Medicine of Universitas Muhammadiyah Sumatera Utara. Additionally, signed informed consent has been obtained for both the procedure as well as the writing and publication. This study adhered to the Helsinki Declaration, the Seven WHO Standards, and the CIOMS Guidelines.
3. RESULTS AND DISCUSSION
PHN is a chronic complication following the reactivation of the VZV that causes HZ. A sharp, burning sensation persists for months after the initial rash appears on the corresponding dermatomes, categorizing PHN within neuropathic pain conditions. Its impact on quality of life prompts affected individuals to seek immediate relief, given the potential to give rise to non-pain symptoms, primarily from a psychiatric perspective. These symptoms include depression, anxiety, social isolation, insomnia, and decreased appetite [9, 10]. Identifying PHN as both an economic and public health burden was an ideal decision, given the array of pain-relieving options available. However, it is crucial to acknowledge that medication-based strategies, while diverse, may entail the risk of adverse reactions in certain instances [11].
This case report has presented the condition of a patient with some remarkable complaints of daily life disturbance, as previously outlined. The patient described their day as extremely unsatisfactory, accompanied by a persistently gloomy mood. The impact of pain experienced was undeniable, registering at a severity level of 5-6/10, elevating to 9-10/10 in response to exacerbating events, such as light, touching solid things, or specific clothing. Furthermore, there was a substantial decrease in productivity, as it was harder to focus or concentrate on a task due to minute-by-minute thoughts of pain. Despite a combination of analgesic agents, the efficacy proved insufficient, necessitating continuous drug consumption as the effect diminished by hours. The medication history of the patient included opioids, tramadol, pregabalin, etoricoxib, and paracetamol, listed in chronological order from the most recent agent to the oldest. Following a recent joint-referral system by a neurologist and internist with opioid administration, several events of constipation and dizziness were apparent, further worsening emotional status alongside pain-related burdens.
The need for a novel pain relief approach for PHN has been extensively discussed. While the evidence supporting TPVB remains under scrutiny, it shows promising potential. To exemplify the current status, this study has reported the case of a patient with VAS around 7-8, which subsequently reduced to 1 after 2 weeks of the first procedure. According to a study by Makharita et al., a single TPVB may significantly attenuate pain in the acute HZ with a basal pain level of 7.37 ± 1.57 out of 10 in the active group. By the third week, it reduced to 0.5 ± 1.41 out of 10, and in the fourth week, it reduced to 0.46 ± 1.29 out of 10. Despite the overall pain scale not differing beyond that time point, the single TPVB group had a lower rate of developing PHN after 3 months (11.4% vs. 22.1%; P=.094), suggesting a potential preventive effect. Additionally, it could reduce the total need for both pregabalin and/or acetaminophen over 24 weeks of follow-up [6]. A meta-analysis by Kim et al. also described that the procedure significantly decreased the incidence of PHN even after a year of post-rash eruption. Continuous or repeated procedures have been reported to be expected to convey lower incidence [12].
Dexamethasone, administered perineurally at a dose of 10 mg, serves as an adjuvant for local anesthesia in this novel approach. As a potent synthetic corticosteroid, it possesses anti-inflammatory effects 7 times more potent than prednisolone, with minimal mineralocorticoid activity and a half-life of approximately 36 to 54 hours. While the exact mechanism is not fully understood, dexamethasone is believed to alter the inflammatory response and may directly affect nociceptive fibers. The perineural administration of this drug exerts effects through several mechanisms, including inhibition of inflammatory mediators and reduction of ectopic discharge from neurons. Widely acknowledged for enhancing the quality and duration of peripheral nerve blocks when combined with local anesthesia, dexamethasone prolongs its analgesic effect by inducing vasoconstriction, reducing the absorption of local anesthesia, or increasing the inhibitory activity on potassium channels in nociceptive C-fibers. This action diminishes nociceptive fiber activities, extending sensory and motor blockade [13-15].
Wang et al. applied a modification to the TPVB procedure by adding Methylene Blue (MB), an inhibitor of nitric oxide synthesis to the injected solution. The study aimed to amplify analgesic and anti-inflammatory effects, with favorable results observed in both arms. MB group disclosed better outcomes, showing the potential of this modification to enhance the efficacy of TPVB [16]. Similarly, Zhao et al. conducted a single-arm study showing that US-guided MB TPVB procedures may offer remarkable pain relief for up to a month or even longer. The reported pain scale at the last follow-up checkpoint was 1.5 ± 1.4 [17].
Based on the explanations above, the effectiveness of TPVB in HZ varies. While this procedure has been explored as a potential intervention for acute pain relief in HZ, some studies suggest significant pain attenuation in the early stages. However, certain results showed that the overall pain scale differed significantly beyond a particular time point, presenting potential limitations in long-term pain relief. It is important to acknowledge that the effectiveness of TPVB varies among individuals. Therefore, more investigation is needed to establish its long-term benefits and preventive effects for PHN. In this context, the application of this approach in the presented case served as a pain reliever, thereby improving the quality of life of the patient.
CONCLUSION
In conclusion, this case report has provided a comprehensive overview of the status of the TPVB approach in attenuating neuropathic pain due to PHN in Indonesia. The results have shown the procedure to be efficacious. A larger group of analyses should be conducted to confirm the true efficacy of TPVB in either preventing or treating PHN.
LIST OF ABBREVIATIONS
| PHN | = Post-herpetic Neuralgia |
| HZ | = Herpes Zoster |
| USG | = Ultrasonography |
ETHICAL STATEMENT
Ethical approval was received from the health research ethics committee of the Faculty of Medicine of Universitas Muhammadiyah Sumatera Utara (approval no.: 663.A.KEPK/FKUMSU/2021). This study adhered to the Helsinki Declaration, the Seven WHO Standards, and the CIOMS Guidelines.
CONSENT FOR PUBLICATION
A signed informed consent has been obtained for both the procedure as well as the writing and publication.


